Defense Cells in the Tissue: Macrophages, Dendritic Cells, and Mast Cells
Macrophages, dendritic cells, and mast cells serve as key defense cells in tissues, bridging innate immunity by detecting threats, engulfing pathogens, and coordinating adaptive responses.
1. Macrophages
Macrophages are large, powerful phagocytes that act as the body's primary cleanup crew.
Function: They identify, engulf, and digest cellular debris and pathogens through a process called phagocytosis.
Role in Signaling: After "eating" a pathogen, they release cytokines that cause inflammation and recruit other immune cells to the site of infection.
2. Dendritic Cells
Dendritic cells are the vital bridge between the innate and adaptive immune systems.
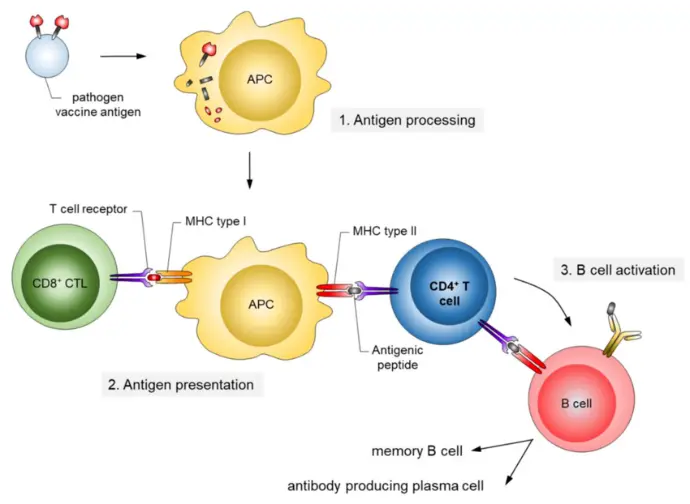
Function: They are specialized Antigen-Presenting Cells (APCs). They capture parts of a pathogen (antigens), travel to the nearest lymph node, and "show" these antigens to T cells.
The Link: Without dendritic cells, your B cells would not be efficiently activated to produce the antibodies described above.
3. Mast Cells
Mast cells are best known for their role in allergy and wound healing. They are packed with granules containing inflammatory chemicals.
Function: When they detect a threat (or an allergen), they undergo degranulation, releasing histamine and heparin.
Impact: This causes local blood vessels to dilate and become "leaky," allowing other defense cells to move from the blood into the tissue quickly.

Cytokines and Chemokines
Immune cells don't work in isolation; they use chemical "text messages" to coordinate an attack.
Cytokines: These are signaling proteins (like Interleukins) released by Macrophages and Dendritic cells to activate other cells.
Chemokines: A specific type of cytokine that acts as a GPS coordinate, guiding circulating white blood cells from the blood vessels directly to the "battlefield" in the tissue.
Antigen Presentation
Antigen presentation displays processed antigen fragments on major histocompatibility complex (MHC) molecules at the cell surface to activate T cells in adaptive immunity.
MHC Class I Pathway
All nucleated cells present endogenous antigens (e.g., viral or tumor proteins) via MHC I. Cytosolic proteins degrade into peptides by the proteasome, then transport via TAP into the endoplasmic reticulum for MHC I loading and surface expression to CD8+ cytotoxic T cells.
MHC Class II Pathway
Professional antigen-presenting cells (dendritic cells, macrophages, B cells) handle exogenous antigens from endocytosis or phagocytosis. Peptides form in endolysosomes, load onto MHC II after invariant chain removal, and present to CD4+ helper T cells.